I wrote the following articles published in November 2016 by the Children’s Hospital of Philadelphia Research Institute:
Tag: psychology
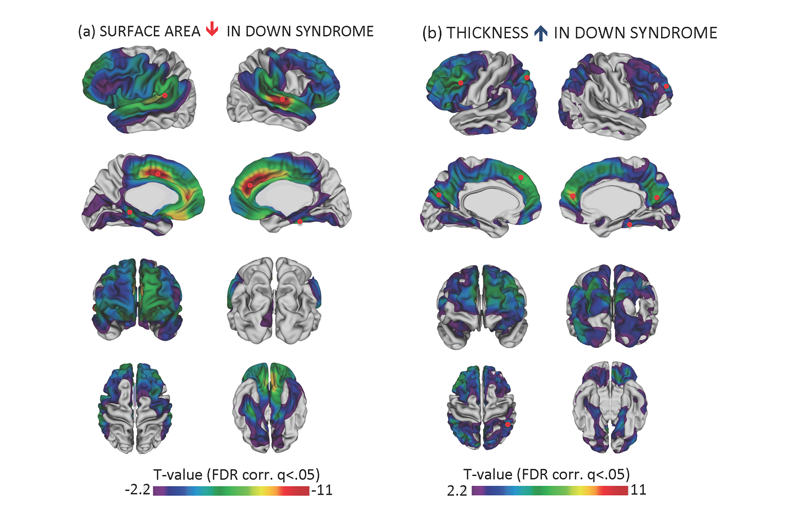
Thick Cortex Could Be Key in Down Syndrome
Originally posted on DrexelNow.
The thickness of the brain’s cerebral cortex could be a key to unlocking answers about intellectual development in youth with Down Syndrome. It could also provide new insights to why individuals with this genetic neurodevelopmental disorder are highly susceptible to early onset Alzheimer’s Disease later in life.
(more…)

Why Diet Apps Fail
Drexel News Blog It’s actually not complicated at all. The reason most smartphone diet apps fail has nothing to do with the diet, and little to do with the app. A team of Drexel researchers is working on a solution to the real problem: getting … Continue reading Why Diet Apps Fail
Mapping Language in the Brain

The exchange of words, speaking and listening in conversation, may seem unremarkable for most people, but communicating with others is a challenge for people who have aphasia, an impairment of language that often happens after stroke or other brain injury. Aphasia affects about 1 in 250 people, making it more common than Parkinson’s Disease or cerebral palsy, and can make it difficult to return to work and to maintain social relationships. A new study published in the journal Nature Communications provides a detailed brain map of language impairments in aphasia following stroke.
(more…)
How to Harness the Science of Sparking Ideas
Originally posted on DrexelNow.
When you say “aha!” at the spark of a surprising new idea or creative solution to a problem, the idea seems to come out of nowhere. But when such insights pop up without your conscious awareness, how can you train your brain to deliver more of them?
Creative ideas tend to come to people all of a sudden, sometimes in the shower or, famously in the case of Archimedes, who shouted “Eureka!” and ran naked through the streets of ancient Syracuse, in the bath. But, like all ideas, they originate in the brain.
For Drexel psychology professor John Kounios, PhD and his longtime collaborator Mark Beeman, PhD, at Northwestern University, the brain science of “aha! moments” has been a major focus of their careers. In 2004, the pair sprang to international acclaim with their discovery that “aha moments” originate in a key spot of the brain’s right hemisphere just above the right ear—putting to rest the question of whether sudden insight was indeed a separate form of problem-solving from more deliberate analytic processes. For the next decade, they’ve continued to refine their studies of how creativity, especially sudden insight, works in the brain and in practice.
Now, the two have co-authored a new book bringing that science to life and offering a comprehensive picture of the state of scientific knowledge about insight: “The Eureka Factor: Aha Moments, Creative Insight, and the Brain” (Random House, 2015). It’s the first book about creativity that tells a complete and faithful story of the neuroscience written by the actual scientists who made the discoveries.
The book is packed with anecdotes about creative insights—from character design at Disney Pixar to a concert promoter tasked with pleasing Elvis Presley—taking each story as an object lesson in the ways creativity works in the brain, according to the latest research.
The book also highlights numerous examples and recommendations of techniques to improve creativity—but, Kounios notes, such recommendations must be used with care. Factors including sleep, mood, motivation and working environment can all affect insight and can be modified to inspire more creativity, if handled with appropriate knowledge of what to do.
“There are strategies to be more creative, but you have to understand the process in the brain to use them correctly,” said Kounios, who directs Drexel’s doctoral program in applied cognitive and brain sciences in the College of Arts and Sciences. “Otherwise, the strategy can have opposite of your intended results.”
For example, Kounios noted that a positive mood often enhances creativity—but not if a person is perpetually sunny. “Creativity requires multiple perspectives, so you need something to jar you out of that state of mind, even if it happens to be sad.”
– See more at: http://drexel.edu/now/archive/2015/March/Creative-Insight-Eureka-Factor/#sthash.V7Ai5bCg.dpuf

Five Questions You Should Ask When Choosing a Therapist
Drexel News Blog Drexel’s Psychological Services Center serves clients of all ages from across the Philadelphia region. Seeking care for behavioral health concerns, whether for yourself or your child, can itself cause some stress – especially if you don’t know what to look for in … Continue reading Five Questions You Should Ask When Choosing a Therapist
Psychological Services Center Opens at Drexel, Offering Affordable, Cutting-Edge Care for Philadelphia Region
Originally posted on DrexelNow.
A new center on Drexel University’s campus in the University City section of Philadelphia is now offering high-quality, scientifically informed, affordable psychological services to clients of all ages from the city and surrounding region.
The Drexel Psychological Services Center offers assessments and therapy provided by doctoral students in Drexel’s highly competitive clinical psychology PhD program, who are working as trainees under the supervision of licensed professional faculty from the Department of Psychology in the College of Arts and Sciences.
Drexel will formally celebrate its opening at a ribbon-cutting ceremony on Oct. 2.
“A real advantage of coming to Drexel’s Psychological Services Center is that we offer the newest evidence-based assessments and treatments,” said Jennifer Schwartz, PhD, director of the center. “These services have undergone scientific evaluation to demonstrate that they are effective, and are not always available in community practices.”
Most services at Drexel’s Psychological Services Center are offered on a sliding fee scale and medical insurance is not accepted. Fees are typically set to be manageable for clients and depend on the size and income level of the client’s household. The center welcomes members of the surrounding communities and students at other universities, but encourages full-time Drexel students to continue to use the University’s Counseling Center, free of charge.
The center’s areas of specialty align with those of Drexel’s psychology faculty, including:
- Mood and anxiety disorders, including evidence-based treatments for stress, depression, anxiety, phobias, trauma, grief, relational issues and identity concerns
- Disorders of eating, including anorexia, bulimia, compulsive overeating and weight management, bariatric surgery evaluations
- Behavioral medicine, including evidence-based approaches to stress management, sleep disorders, concerns related to reproductive health and living with chronic pain or other physical health problems
- Clinical neuropsychological assessments including services for attention and executive functioning, learning and memory, concussion and mild traumatic brain injury and other neurological injuries and diseases
- Child and adolescent services including evidence-based treatments and assessments for behavioral concerns such as ADHD, mood problems, social skills challenges, academic and school challenges, health risk behaviors and more
- Forensic psychological assessments, including assessments of intellectual ability and adaptive function for justice-involved individuals
As a training facility for Drexel’s doctoral students, the Psychological Services Center offers many advantages to clients as well as to the trainee clinicians. Clinicians carry small caseloads and are able to devote a great deal of attention to each client. Clinicians are closely monitored by, and meet regularly with, their experienced supervisors to ensure they are delivering the best possible care.
Individuals interested in seeking services at Drexel’s Psychological Services Center should call 215.553.7128 to schedule a no-cost intake appointment to determine if the center is a good fit.
For more information about the Psychological Services Center, visit the clinic website.
– See more at: http://drexel.edu/now/archive/2014/September/Psychological-Services-Center-Opens/
First Study Asks Autistic Adults about Driving Experiences
Originally posted on DrexelNow.
In the first pilot study asking adults on the autism spectrum about their experiences with driving, researchers at Drexel University found significant differences in self-reported driving behaviors and perceptions of driving ability in comparison to non-autistic adults. As the population of adults with autism continues growing rapidly, the survey provides a first step toward identifying whether this population has unmet needs for educational supports to empower safe driving – a key element of independent functioning in many people’s lives.
“Previous research in my lab has included extensive research in driving capacity with people who have a variety of conditions such as multiple sclerosis or who had experienced traumatic brain injury,” said study co-author Maria Schultheis, PhD, an associate professor of psychology at Drexel. “When we investigate whether and under what circumstances a condition or neurological difference might affect driving ability, as a standard starting point we want to go to individuals and find out from their perspective what problems they are having on the road, in their real-world experience. That question is pivotal to shape and inform the goals of long-term research – and is especially important when we turn to look at a developmental difference like autism, where there has been too little research to establish yet whether widespread driving difficulties exist.”
Only a few previous studies have examined driving ability in individuals with autism, and those studies focused on adolescents and new drivers rather than experienced adult drivers. These studies relied on parent surveys and evaluations of discrete aspects of driving performance. The new Drexel study, published early online this month in the Journal of Autism and Developmental Disorders, used a validated survey that has been extensively used in driving research, and asked adult licensed drivers on the autism spectrum to describe their first-hand, real-world driving experiences.
“We were beginning to see discussion in the research literature that aspects of autism spectrum disorders, such as neurocognitive challenges and social recognition difficulties, could make it likely that members of this population would experience significant challenges with driving,” said the study’s lead author Brian Daly, PhD, an assistant professor of psychology in Drexel’s College of Arts and Sciences. “But that assumption hadn’t been studied in adult drivers, or based on the experiences of the drivers themselves – so these were the questions we explored.”
In this survey, adults with autism spectrum disorders reported earning their drivers’ licenses at a later age, driving less frequently and putting more restrictions on their own driving behaviors (such as avoiding driving on highways or at night), on average compared to non-autistic adults. The respondents with autism spectrum disorders also reported more traffic violations.
Because this pilot study was relatively small and based on self-reports of 78 ASD respondents and 94 non-ASD comparison participants, Schultheis and Daly noted that the differences they found were open to several possible interpretations. Autistic adults may have reported driving less often and restricting their behaviors out of self-awareness of actual difficulties or deficiencies in their driving. These difficulties and/or reduced driving exposure could also explain the higher rate of reported violations.
Alternatively, it is possible that the respondents on the autism spectrum were more honest in their answers, but no worse at driving than everyone else.
“In driving research, it’s well established that people have a positive bias when reporting their own driving skills,” said Schultheis. “Because the study relied on self-reported answers, we can’t rule out whether the respondents with autism were simply being more descriptive and honest about their difficulties than the control group.”
One intriguing finding that Daly and Schultheis noted was that the difficulties adults with autism reported were not clustered in any specific areas, such as problems related to social processing of other drivers’ or pedestrians’ expected behaviors, or difficulties with neurocognitive aspects of driving such as motion perception and reaction time.
“It suggests that the challenges these individuals are facing are more global than specific,” Daly said.
“This is such an important study,” said Paul Shattuck, PhD, an associate professor and director of the research program area in life course outcomes at the A.J. Drexel Autism Institute, who was not involved in conducting the study. “Cognitively-able adults on the autism spectrum face many barriers to full participation in society. Facilitating access to transportation options will increase the capacity for these adults to contribute to their communities.”
Daly and Schultheis are continuing to investigate driving behavior in adults with autism through further research, with funding from the A.J. Drexel Autism Institute, the first autism research center focused on a public health science approach. In the next phase of research, the team is using driving simulation in Schultheis’ lab to objectively capture aspects of actual driving performance in adults on the autism spectrum. Individuals interested in enrolling in these studies should contact schultheis@drexel.edu.
“This is a first step toward identifying, categorizing and quantifying challenges that may exist in this population,” Schultheis said. “What we find will help determine what needs there may be for interventions, from driver education programs to different kinds of training exposures.”
– See more at: http://drexel.edu/now/archive/2014/June/Autism-Driving-Study/

How a Web-Based Questionnaire Can Help Prevent Teen Suicide
Drexel News Blog Getting teenagers to talk about what’s bothering them isn’t always easy. But with new guidelines from the American Academy of Pediatrics recommending depression screening for adolescents (ages 11-21) during their annual physical, getting teens talking at the doctor’s office is a must. … Continue reading How a Web-Based Questionnaire Can Help Prevent Teen Suicide
New Mobile App and Talk Therapies for Binge Eating Disorder
Originally posted on DrexelNow.
Two new treatment methods under investigation at Drexel University aim to help people reduce binge-eating behavior.
A smartphone app in development will track users’ individual patterns of eating and binge eating behavior and alert them at times when they are at risk for binge behaviors, among a comprehensive suite of other features.
Another treatment is a new, evidence-based approach to small-group behavioral therapy that will equip patients with psychological tools that may help them adhere to, and benefit from, standard treatments for binge eating disorder.
Binge eating disorder, characterized by periods of eating objectively large amounts of food, is “associated with a great deal of clinical distress,” said Dr. Evan Forman, an associate professor of psychology in Drexel’s College of Arts and Sciences, co-director, with Dr. Meghan Butryn, of the Laboratory for Innovations in Health-Related Behavior Change, where both studies are being conducted.
Binge eating disorder, only recently identified as an official diagnosis in the Diagnostic and Statistical Manual of Mental Disorders, was found to be about twice as common as bulimia nervosa in a large international survey published earlier this week.
People who engage in binge eating behavior may feel ashamed, out of control and isolated because they may not know others with the disorder, or even know they have a clinically recognized disorder.
The most scientifically supported treatment, cognitive behavioral therapy (CBT), leads to remission for only between 50-60 percent of individuals who complete a full course of treatment.
“It could be improved,” Forman said. “These two studies are an attempt to improve treatments for binge eating.”
A Mobile App for Binge Eating Disorder
Among binge eaters, “there is a cycle of sorts – mounting pressure toward a binge episode, with certain triggers that make it more likely that a binge episode will occur,” Forman said. With cognitive behavioral therapy, a clinician helps patients recognize their personal triggers and learn to interrupt them.
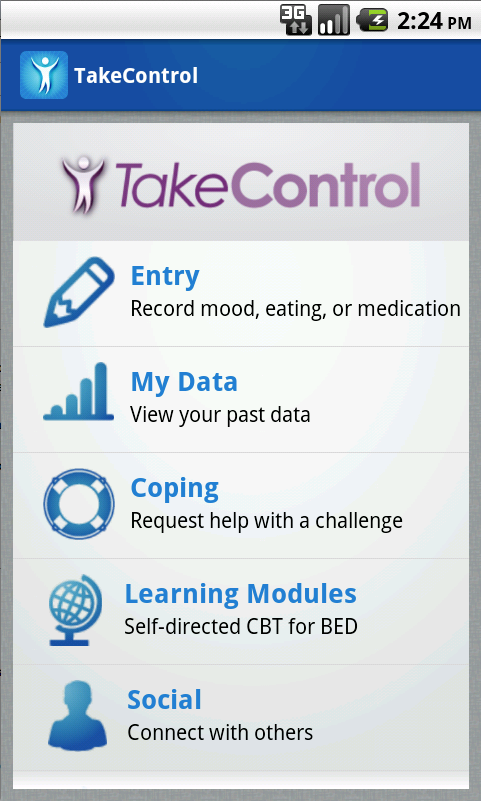
Forman’s lab is developing the “TakeControl” mobile phone app to provide a similar help right in the patient’s pocket – and in real time, at the moment the trigger occurs.
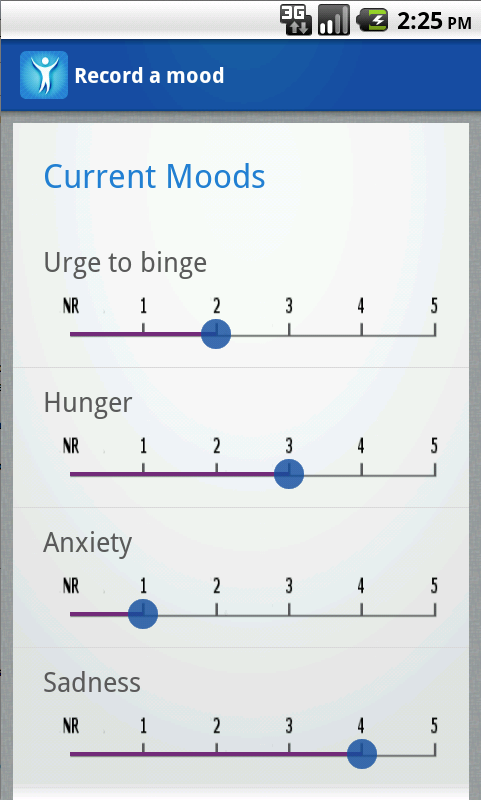
In the app, users can record their binge-eating activity and urges, multiple mood states and whether or not they’ve eaten regular meals and taken their prescription medications. As the app learns about an individual’s patterns of binge-eating behavior and their individual triggers, it can prompt the person with a warning alert when their personal risk is high.
“It could be an emotion like rejection, loneliness, sadness or anxiety, or something external such as passing a certain convenience store, or a time of day or night,” said Forman, who is the principal investigator of the project.
When warned that they are at risk for a binge, or at any time of their own choosing, users can follow the app’s customized interventions to help them in the moment when they need it.
Users of the “TakeControl” app can choose how much and how little of their personal data to enter to help the app help them. The app also includes learning modules, optional personal goal-setting modules and optional social networking features to connect with others who share this often-isolating disorder.
“Using the data visualization modules, people can chart their behavior patterns over time,” said Stephanie Goldstein, a graduate student in Forman’s lab working on the project. “This shows people the progress they’ve made and reinforces it. Someone could also learn from the charts, for example, how their binges relate to their anxiety.”
Forman’s research team is developing the app on the Android platform in collaboration with the Applied Informatics Group in Drexel’s College of Computing and Informatics.
“Most users have their smartphone with them upwards of 20 hours a day, so a mobile app can be a very effective way to monitor behaviors that a physician wouldn’t automatically know about,” said Gaurav Naik, a co-investigator on the project from the AIG. “By combining AIG’s knowledge of engineering systems that can learn from data, and the clinical knowledge of our partners in psychology, we can develop an app that we hope can generate successful outcomes.”
The project was one of two winners selected in an internal university-wide competition under the auspices of a Shire Pharmaceuticals-Drexel University Innovation Partnership. In December 2013, each project will be considered by Shire for further expansion and commercialization. If funded, the group expects to also develop a version for iOS.
Future plans for the app include connections with other technologies for automatic personal data tracking, such as smart pill bottles, web-connected scales and activity bands, as well as existing popular diet and fitness-tracking apps.
Users of the app will also have the option to share their data with their therapist or other clinician, either automatically through a clinician’s portal, or by bringing their exported data to a therapy session.
Therapy to Help the Therapy Work Better
“Standard treatment for binge eating disorder is largely behavioral – in that it tells people what to do,” said Dr. Adrienne Juarascio, a postdoctoral fellow in Forman’s lab who is the principal investigator of the in-person treatment study. “In CBT we ask people to adhere to uncomfortable treatment recommendations, such as eating every three to four hours even when they are concerned about weight gain. Or they might be asked to engage in alternative activities while they are having the urge to binge.
“It can be very difficult to complete these treatment recommendations, no matter how motivated people are.”
Juarascio is now coordinating an experimental treatment program for binge eating disorder that teaches patients psychological strategies to deal with the discomfort associated with traditional treatments.
The 10-session group therapy program integrates the gold-standard cognitive behavioral therapy with another method, acceptance and commitment therapy (ACT) and other third generation acceptance-based behavioral treatments, to help patients learn to tolerate and accept stressful experiences and distressing thoughts, without engaging in disordered behaviors.
“Different people find it uncomfortable for different reasons,” Forman said. “For example, if someone had binged the night before and thought, ‘There’s no way I’m eating breakfast after that,’ the ACT skills are designed to help the person recognize this feeling of being repulsed by food, and proceed to eat breakfast anyway because consistently eating regular meals is healthier in the long run.”
Juarascio previously piloted the approach, combining treatment-as-usual with ACT in the treatment of eating disorders more broadly, as part of her doctoral research at Drexel. In the July 2013 issue of the journal Behavior Modification, she, Forman and other colleagues reported that patients receiving the combined therapy had better outcomes at a six-month follow-up than did those receiving standard treatments.
– See more at: http://drexel.edu/now/archive/2013/September/Binge-Eating-Smartphone-App-Therapy-Studies/